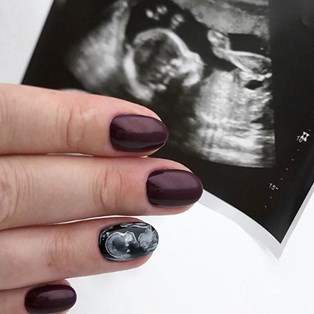
Nuchal translucency: NT scans and what they mean
Everything you need to know
By Gina Flaxman
May 24 2019
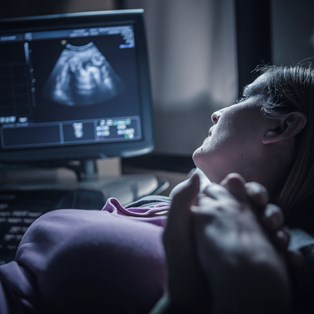
Throughout your pregnancy, there are several tests and scans available. The nuchal translucency scan (NT scan) is an ultrasound that may detect the risk of some chromosomal abnormalities in the foetus.
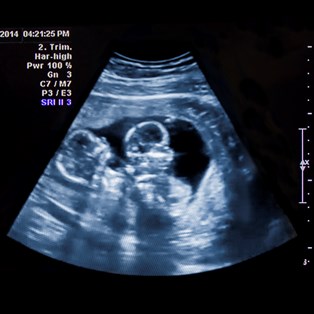
Nuchal translucency is a collection of fluid under the skin at the back of the baby’s neck. It can be measured between 11 and 13 weeks of pregnancy or when your baby measures between 45-84mm.
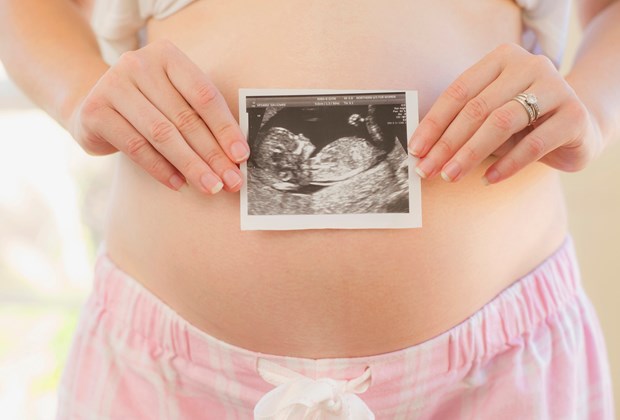
You don’t have to have an NT scan but most women choose to have it as part of their 12-week ultrasound. If you decide to have the scan, the ultrasound technician will measure the nuchal fold thickness at the back of your baby’s neck. The scan is usually done through your abdomen but occasionally a probe will need to be inserted into the vagina. Women with twins or multiple births can also have the scan but the results are not as accurate.
The results of the measurement will tell you whether your baby has a high or low risk of a chromosomal abnormality such as Down syndrome, Edwards syndrome or Patau syndrome. Increased thickness may indicate an abnormality but it can’t tell you definitively whether or not your baby has an abnormality.
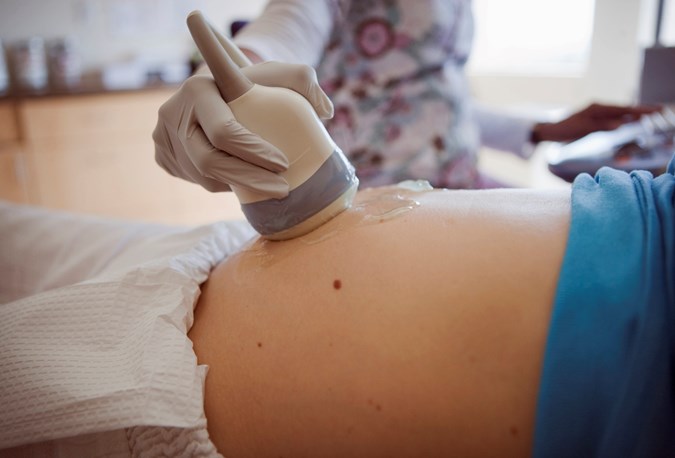
Getty Images
What do the results mean?
An NT measurement of less than 3.5mm is considered normal. As the NT increases, so does the risk of your baby having chromosomal abnormalities. But it’s important to note the test only measures the risk and is only one test. Some babies with increased fluid don’t have Down syndrome or any other abnormality.
Combined test
The result of your NT scan is usually combined with other test results. The risk calculation is also based on the mother’s age, the baby’s gestational age and nasal bone, and blood tests.
The blood test measures the levels of the hormone hCG and the protein PAPP-A. Babies born with Down syndrome tend to have high levels of hCG and low levels of PAPP-A. When the NT scan is combined with a blood test the detection rate increases to 90 per cent.
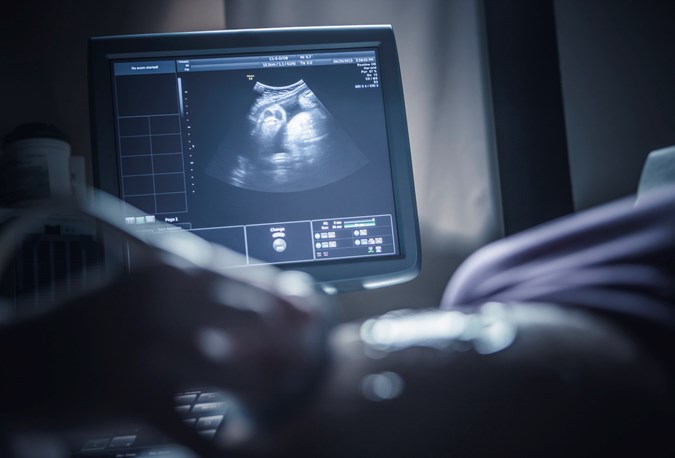
Getty Images
What if your baby is high risk?
If your risk is less than one in 1000 you are considered low risk. If your risk is between one in 50 and one in 1000 you are considered intermediate risk. If the risk is greater than one in 50 it is considered high risk.
With this results chart, it’s important to remember that even if your baby is classified as high risk there is still a good chance they don’t have a chromosomal abnormality. You may be referred to a genetic counsellor to discuss your options.
You can decide whether or not to have a more invasive diagnostic test, such as chorionic villus sampling (CVS) or amniocentesis.
These tests can tell you definitively whether or not your baby has a chromosomal abnormality but they carry a small risk of miscarriage. You can have CVS from 11 weeks of pregnancy and an amniocentesis from 15 weeks.

Getty Images
Non-invasive prenatal testing
A non-invasive prenatal test (NIPT) is a relatively new, highly sensitive blood test that screens for Down, Edwards, Patau and Turner syndrome. In Australia, it has only been available in some private, specialist centres in the past five years.
Sometimes referred to by the names of the companies that produce them, such as Harmony, Percept and Generation, the test can be done from 10 weeks of pregnancy. It analyses the genetic information in the baby’s DNA, some of which passes into the mother’s bloodstream during pregnancy. It picks up more than 99 per cent of cases of Down syndrome.
But NIPT is still only a screening test. You can only get definitive information with CVS or amniocentesis. NIPT is expensive and not covered by Medicare but it’s a good option if you are at increased risk (you are older or have previously had a baby with chromosomal abnormalities) and you can then decide whether or not to opt for the more invasive tests, which carry the risk of miscarriage.
Some laboratories also test for the baby’s gender and look for problems with the sex chromosomes. So the test can also tell you definitely whether you are having a boy or a girl, if you choose to find out.